Keloids - Medical Condition
Keloids
Keloids Facts
Keloids are benign (noncancerous), fibrous skin tumours. They are most common in people with darker skin (e.g., people from West Africa or Southern India). People usually develop them between the ages of 10 and 30. Men and women are equally likely to have keloids. Keloids may also run in families.
Keloids Causes
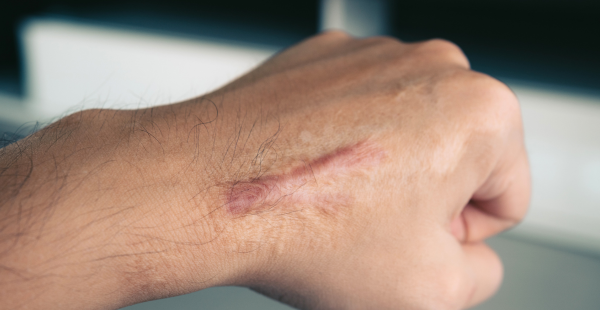
Keloids usually occur at the site of skin damage (e.g., acne, burns, chicken pox, cuts, insect bites, piercings, surgery, tattoos, vaccinations), although they can occur spontaneously. Whether or not a keloid will form is not determined by the severity of the wound – even a minor skin abrasion can result in keloid formation.
Keloids are the result of abnormal wound healing. Normally, there is a balance between the production and the breakdown of collagen, which is a protein that makes up the fibres in the skin. With keloidal scars, the cells in the skin called fibroblasts produce excessive amounts of collagen. The collagen fibres are also thicker and wavier. This leads to the thick, raised appearance that is characteristic of keloidal scars. It is unclear what prompts this unusual healing process. Possible causes include genetic factors, skin tension, and the presence of a very high number of fibroblasts in the skin.
Keloids Symptoms and Complications
Keloids are usually firm, raised, shiny, and smooth. They are often pink or red, or much darker or lighter in colour than the surrounding skin. Keloids always extend beyond the limits of the original wound, sometimes by many centimetres. The colour, shape, and size of the scars may change with time. They are generally not painful, though they are often itchy.
Keloids are more likely to develop on the arms, back, ears, lower legs, mid-chest, and neck. They may form as a wound heals, or they may take several months or even years to develop. Rarely, they will continue to grow indefinitely.
There are generally few complications from keloidal scars. Depending on their appearance and location, they can cause some psychological distress, as keloids can be quite prominent. Keloids can also interfere with movement, especially if they are on a joint. Very rarely, keloids may become cancerous.
Keloids are different from hypertrophic (abnormally thickened) scars in that they extend beyond the edges of the site of injury and can occur without any inciting injury. Hypertrophic scars are more common than keloids, and many people who think that they have keloids actually only have a tendency towards hypertrophic scarring. Your doctor can help make this distinction.
Making The Keloids Diagnosis
Keloids can be diagnosed by your doctor or dermatologist (skin specialist). Diagnosis is based on the location and appearance of the scar, and how it progresses over time. Your doctor may do a physical exam and look at your medical and personal history to rule out any other possible diseases or conditions. A skin biopsy may be performed to confirm the diagnosis and to rule out any malignant tumor.
Keloids Treatment and Prevention
Currently, there is no completely effective way to treat keloids or to prevent their formation. Traditionally, surgical removal of the scars was recommended. However, 45% to 100% of people will have a recurrence of the scar if surgery is not combined with other treatment (e.g., radiation, pressure dressings), and the new scar can actually be larger and more prominent than the original scar.
A mainstay for both treatment and prevention is the injection of steroids such as triamcinolone directly into the scar. Steroids help prevent inflammation and promote the breakdown of collagen. This helps to make scars less raised, and to decrease pain and tenderness associated with the scar.
Laser therapy is now used to treat many types of skin problems, including keloids. It is often combined with steroid injections to give the best cosmetic result.
Silicon gel dressings are a popular alternative to steroid injections, although there is only limited evidence suggesting the dressings are effective in preventing abnormal scarring in people who are at high risk of developing keloids. Other treatment options include radiation therapy and medications such as interferon*, 5-fluorouracil, imiquimod, and bleomycin.
If you have a history of forming keloids and are having surgery, discuss with your surgeon any strategies to prevent keloid formation. Also, those with a tendency to form keloids may want to avoid any unnecessary piercings or surgeries.
All material copyright MediResource Inc. 1996 – 2026. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/condition/getcondition/Keloids
