Cellulitis - Medical Condition
Cellulitis
Cellulitis Facts
Cellulitis is a serious infection that spreads under the skin, affecting soft tissues such as the skin itself and the fat underneath it. Bacteria are the most common culprits, but very occasionally a fungus is responsible.
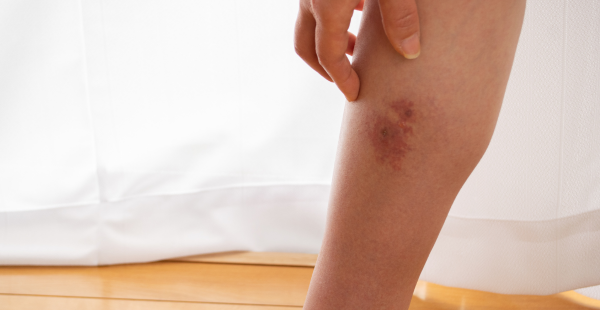
Cellulitis is not contagious, but it can strike anyone with broken skin or damaged tissue. Cellulitis infections occur most commonly on the legs, arms, or face. Facial infections are found mostly in infants and seniors.
Cellulitis occurs in different forms. Periorbital cellulitis occurs around the eye sockets. Erysipelas results in raised, firm, bright red patches of skin and is caused by Streptococcus bacteria. Necrotizing fasciitis is an infection that occurs below the skin.
Cellulitis Causes
Cellulitis usually starts with a break or tear in the skin. Many species of bacteria inhabit the skin’s surface and can thrive underneath it if the barrier is broken to let them through. Bacteria can infect burns and bruises as well as cuts and scratches, puncture wounds, and dermatitis. Other traumas that can lead to infection include:
- surgery
- dental work
- animal or human bites
- injection drug use
There are several bacteria that can cause cellulitis. Streptococcus and Staphylococcus are the two most common species. The actual type of bacteria causing the infection depends on the nature of the exposure, such as infections resulting from a cut, a cat or dog bite, or swimming in salt or fresh water with broken skin.
Cellulitis can sometimes start even on skin that hasn’t been broken. This normally only occurs in people with weakened immune systems. People with diabetes, people with alcoholism, people taking corticosteroids, and others with compromised immune systems are at greatly increased risk of cellulitis and tend to get worse infections.
Necrotizing cellulitis (or necrotizing fasciitis), a rare but severe form of cellulitis, is the dreaded "flesh-eating disease" that occasionally grabs media headlines. There are 2 types. The first is due to a very aggressive strain of Group A streptococcus and can start anywhere on the skin. The second is due to a polymicrobial infection of different bacteria that often starts just forward of the anus following surgery or rectal abscesses. Necrotizing cellulitis starts as an extremely painful, red swelling that soon turns purple and then black as the skin and flesh die. However, the risk of getting necrotizing cellulitis is extremely small. The risk is a bit higher for people who are already sick or have a compromised immune system.
Cellulitis Symptoms and Complications
Uncomplicated cellulitis begins with a small area of skin that’s red, glossy, painful, and warm to the touch, typically around a cut. It most often strikes the lower leg, but the arms, hands, feet, and groin are other likely sites.
Some types of bacteria can get into the lymphatic system, a network of tubes and nodes that carry disease-fighting cells and waste matter around the body. If this happens, the infection can travel under the skin and spread to other parts of the body.
Another type of cellulitis is erysipelas. The inflamed skin in erysipelas is not smooth but raised, often completely separated from the layer beneath by a pocket of gas created by the bacteria. There’s often a fever a day or two before the rash.
The most severe complications of cellulitis are meningitis and blood poisoning (if the bacteria get into the bloodstream, called bacteremia). Meningitis can occur if the bacteria get inside the central nervous system (e.g., brain or spinal cord). The most likely route is through the eye socket. Cellulitis around an eyelid is called preseptal cellulitis. It causes a rash that might be painful or itchy. If the bacteria get behind the seal where the eye meets its socket, the condition is called orbital cellulitis. This is a medical emergency that causes symptoms of fever and impaired vision. It requires immediate treatment to prevent meningitis or eye damage.
If the infection gets into the lymphatic system or the bloodstream, red lines may be seen under the skin before the main rash appears. This may cause symptoms like fever, sweats, and nausea.
Making The Cellulitis Diagnosis
A doctor can usually recognize cellulitis from the skin’s appearance. Unless there’s pus or an open wound, the responsible organism can be hard to identify. The exact strain of the bacteria isn’t usually important, as typical "broad spectrum" antibiotics will deal with most bacteria that cause cellulitis infections.
Cellulitis Treatment and Prevention
Several types of antibiotics are used to treat cellulitis. The type of antibiotic prescribed will depend on the cause and severity of the infection and on other medical conditions. Uncomplicated cellulitis should start to clear up in just a few days. It’s important to finish the prescribed medication even if the symptoms go away.
When antibiotic treatment begins, your doctor may tell you to restrict movement of the affected area and rest in bed until the infection begins to subside and any fever goes down. Once the infection starts to improve, normal activities can be resumed. Elevating the affected area so that it’s higher than the heart will reduce swelling and pain. Warm compresses increase the blood flow to help fight infection.
Recently, more cases of cellulitis and other skin infections have been linked to methicillin resistant staph aureus (MRSA). This bacteria was only seen in hospital settings in the past, but people can now be exposed to it anywhere. It usually requires specific types of antibiotics to treat. Your doctor will be able to prescribe the appropriate antibiotic for you if they believe you have MRSA.
Antibiotics alone don’t work fast enough to stop necrotizing cellulitis, so the infected flesh has to be cut away. Sometimes, amputation is the only way to prevent the disease from invading the rest of the body.
To avoid cellulitis:
- Wear protective equipment when playing outdoor sports – soil forced into cuts and scratches is a common cause of cellulitis.
- Wear long sleeves and long pants when hiking in the forest, which helps to avoid scratches and other injuries.
- Don’t go outdoors in bare feet.
- Avoid spending time swimming in salt or fresh water (e.g., lakes, rivers, oceans) with broken skin.
- Keep skin clean with a mild soap and water.
- Clean cuts carefully with soap and antibiotic ointment and change bandages at least daily or whenever the bandage becomes wet or dirty.
- See a doctor for large or infected cuts or wounds inflicted by animals.
All material copyright MediResource Inc. 1996 – 2026. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/condition/getcondition/Cellulitis
